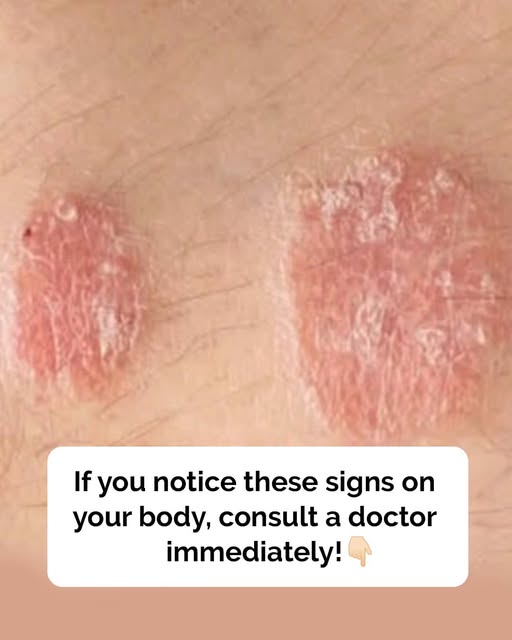
just your skin.
Psoriasis is not a cosmetic inconvenience. It is an autoimmune revolt, a biological betrayal where your immune system accelerates skin cell growth to a frantic pace—cells that should take weeks to mature instead pile up in days, creating the scaly, inflamed plaques that mark over 8 million Americans and 125 million people globally. The Mayo Clinic defines it as a chronic disease causing itchy, scaly patches, but that clinical description fails to capture the 3 AM burning that steals your sleep, the way fabric feels like sandpaper against raw lesions, or the quiet shame of visible flakes on your collar during a meeting.
The National Psoriasis Foundation identifies five distinct manifestations, each demanding a different level of vigilance and carrying its own emotional weight.
Plaque psoriasis, the most common form, presents as raised, red patches coated with silvery-white scales that crack and bleed without warning. These lesions favor elbows, knees, and scalps—territories impossible to hide completely. The thickness varies, but the itch remains constant, moderate to severe, a persistent reminder that your body is fighting itself. On darker skin, the aftermath lingers as post-inflammatory hyperpigmentation, dark shadows that remain long after the active inflammation subsides, creating a secondary battle with discoloration.
Guttate psoriasis strikes suddenly, often in children and young adults following a strep throat infection, scattering small, drop-shaped lesions across torsos and limbs like pink tear stains. Unlike the thick plaques, these spots are thin, less scaly, but no less alarming in their sudden proliferation across previously clear skin.
Inverse psoriasis hides in the body’s folds—groin, buttocks, under breasts—presenting as smooth, shiny, intensely red patches that burn with every step, every friction of fabric, every bead of sweat. This hidden suffering often festers in silence, complicated by fungal infections that thrive in these moist, angry crevices. The location makes it socially isolating, personally humiliating, and physically excruciating.
Then comes the escalation that brooks no delay. Pustular psoriasis erupts with white blisters filled with non-infectious pus, surrounded by skin so inflamed it appears burned. Accompanied by fever and chills, this presentation signals systemic distress, not merely dermatological inconvenience. It requires immediate emergency care.
The rarest and most terrifying is erythrodermic psoriasis, a medical emergency where widespread redness and massive shedding cover the body like a severe burn. Skin loses its ability to regulate temperature and fluid; dehydration and infection become imminent threats. Hospitalization is not optional—it is survival.
But the assault doesn’t stop at skin level. Your nails may thicken, pit like hammered brass, or detach entirely from the nail bed in a condition called onycholysis. These changes often serve as early warning signals of psoriatic arthritis, a companion autoimmune attack that targets joints with the same destructive fury, potentially eroding mobility if ignored.
Understanding these warning signs transforms observation into power. When you recognize the silvery scales, the hidden smooth patches in folds, the sudden drop-like spots, or the crumbling nails, you hold the agency to intervene before irreversible damage takes hold. Your body communicates distress through its largest organ, writing messages in inflammation and pain. Listen without shame. Consult a dermatologist not merely for cosmetic relief, but for the medical management that preserves your sleep, your mobility, your peace of mind, and your fundamental dignity. The mirror reflects not just skin, but a battleground where early recognition saves lives.